Compiled by: Kristina Stiles and Nicholas Goodwin, April 2018
On behalf of the BBA Pre-Hospital Special Interest Group
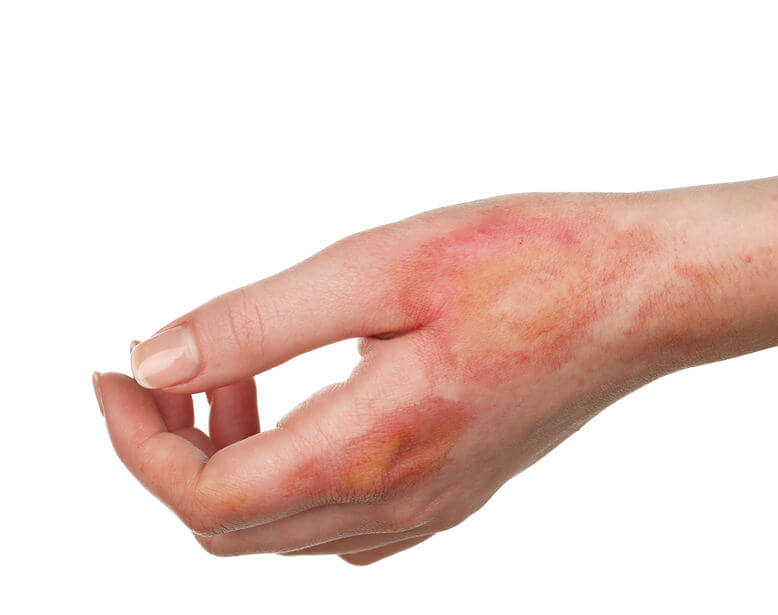
The prompt and effective application of burns first aid has been shown to positively impact on the burn outcome, preventing further tissue damage and reducing subsequent morbidity. However, there is widespread variation in the first aid advice currently available for management of burns and scalds. The following recommendations are based on evidence from a systematic literature review and form a minimum standard of care for first aid management of burns and scalds that is practical and effective to perform in any setting or environment.
Thermal burns
STOP the burning process
Remove person/s from the source of the burn, once safe to do so
- Extinguish burning clothing using water or the ‘Stop, Drop and Roll’ method
STOP where you are
DROP to the ground and cover your eyes and mouth with your hands
ROLL over and back and forth until the flames are out
- Isolate electrical power sources, if safe to do so before attempting rescue
- Avoid chemical cross-contamination
REMOVE clothing and jewellery
- Remove any burned/contaminated/damp/constricting clothing, if able to do so
- Remove any nappies, jewellery and contact lenses near burned area, if able to do so
- Leave any molten/adherent clothing.
COOL the burn
If water is available
- Do not delay cooling.
- Cool the burn immediately with cool running tap water for 20 minutes and within 3 hours of injury
- Aim to complete 20 minutes of cooling. Further cooling attempts may induce hypothermia, especially in children and the elderly, or where large burns are present.
If water supply is limited
- Apply a cool water compress using any clean wetted lint free cloth
- Change compress frequently over 20-minute period
- If no water is immediately available in any form, burns should be covered with cling film and cooled at the first available opportunity within 3 hours of injury.
- Hydrogels are marketed but evidence as to their efficacy is limited
Do not
- Use ice or iced water to cool burns
WARM the patient
- “Cool the burn but warm the patient”
- Keep patient warm to prevent hypothermia (children and elderly are most susceptible)
- Cover non-burned areas during cooling and continue to warm throughout care interventions
COVER the burn
- Cover the cooled burn with loose longitudinal strips of cling film or any clean lint free cloth or non-adherent dressing
- Do not wrap cling film circumferentially around limbs or other burned areas
- Do not apply cling film to facial burns
- Cover irrigated and fully decontaminated chemical injuries with a wet compress
Chemical burns
Immediacy of decontamination and dilution through irrigation of chemical injury is paramount as the duration of the chemical’s contact with the skin is a major determinant of burn severity
Remove chemical agent
- Wear appropriate personal protective equipment to minimize the risk of cross-contamination
- Brush off dry powders, remove fragments of solid chemical substances and discard contaminated clothing prior to wet decontamination1
Irrigate
- Do not delay immediate irrigation for detailed assessment of patient or acquiring a particular irrigation fluid, regardless of delay in presentation.
- Commence urgent irrigation of skin/eyes with a sterile isotonic solution (e.g. Hartmann’s or Normal Saline), an amphoteric solution, or room-temperature running water for at least 20 minutes.
- Continue irrigation until the patient experiences a decrease in pain or burning in the wound or until the patient has been assessed by a burn specialist.
- Do not irrigate dry lime, phenols, muriatic acid, concentrated sulphuric acid and elemental metals with water.
- Do not attempt to neutralize the chemical due to the potential exothermic reaction, which could contribute to further tissue destruction.
Treat
- Access National Poisons Information Service/TOXBASE for agent-specific decontamination and treatment information
- Administer antidote treatment for specific agents if appropriate
- Manage any systemic toxicity or expected side-effects of a chemical agent
Electrical burns
- Prioritise and manage life threatening conditions as per standard ATLS protocol
- Cool the injury site(s) immediately with cool running tap water for 20 minutes within 3 hours of injury (after the electrical source has been controlled)
- If there is no history of unconsciousness, cardiac arrest, or abnormal rate or rhythm (normal ECG), prolonged monitoring is not required.
Tar and Bitumen burns
- Cool the molten agent and the injury site(s) with cool running tap water for 20 minutes within 3 hours of injury or until it is completely cooled
- Once cooled, use solvents containing liquid paraffin or any oily substance to emulsify the tar. Tar removal is not an emergency and may be delayed until arrival at the burn service.
Cold burns (frostbite)
- Prioritise and manage life threatening conditions, such as hypothermia or severe trauma over the presence of regional cold injury.
- In the pre-hospital care of cold injury, begin local rewarming only if refreezing will not occur in transit. Avoid refreezing if field thawing occurs.
- Rewarm rapidly and continually in circulating water at 37°C to 39°C with a mild antibacterial agent (povidone-iodine or chlorhexidine) for at least 30 minutes within 12 hours of injury.
- Rewarming is complete when all injured tissues have regained sensation, feel soft and pliable to the touch, with a red-purple appearance.
- Do not use dry heat as it may compound the injury.
- To avoid further tissue damage, do not apply pressure, massage or rub the affected area
- Elevate the injured area to reduce any developing swelling.